FP for children
FERTILITY PRESERVATION IN CHILDHOOD CANCERS
Diagnosis Of Cancer In Children Is Devastating For Both Children And Their Families. Currently Excellent Survival Rates For Paediatric And Adolescent Cancers Makes Fertility Preservation An Important Component Of Long Term Quality Of Life. Fertility Preservation Options Differ In The Pre And Post-Pubertal Child.
In pre-pubertal children of both genders, fertility preservation entails cryopreservation (freezing) of gonadal tissue, or shielding/re-location of reproductive tissues in the setting of radiation. Pre-pubertal children receiving gonadotoxic treatment may be at risk of delayed or absent pubertal development hence attention to reproductive health should continue after completion of treatment as well.
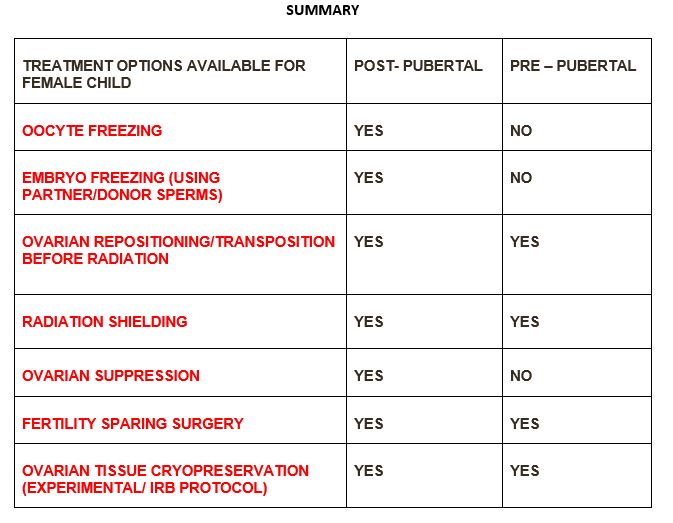
Treatment Options Available For The Female Child
A. EGG (Oocyte) FREEZING
Egg freezing involves harvesting and freezing of unfertilised eggs from the ovary. The patient undergoes a cycle similar to in vitro fertilization (IVF). The process begins with ovarian stimulation using hormones for about 10 days to harvest multiple mature eggs. Next, transvaginal (or, in some cases trans-abdominal) egg retrieval is performed under anaesthesia. The unfertilized eggs are then frozen for future use.
SUCCESS RATES
When ready to attempt pregnancy, the frozen eggs are thawed and fertilized. The resulting embryos are transferred to the uterus of the patient or a surrogate/gestational carrier in case the uterus of the patient is compromised. Egg freezing is no longer considered experimental according to the American Society for Reproductive Medicine. Success rates in young women closely follow those seen with embryo freezing with no increase in the congenital malformation rate. The success of the procedure is directly related to the age of the patient when she froze her eggs and number of mature eggs frozen.
B. EMBRYO FREEZING
Embryo freezing involves the freezing and storing of embryos obtained by ovarian stimulation as a part of IVF process, egg retrieval followed by its fertilisation in vitro in the lab with sperm from partner/donor, and then freezing of embryos for later implantation. This process begins with ovarian stimulation using hormones that are self-injected daily by the patient for about 10 days to harvest multiple mature eggs, followed by a transvaginal retrieval of the eggs under anaesthesia. Sperm used to achieve fertilization can be from a partner or donor.
Note: Ovarian stimulation to cryopreserve eggs or embryos can be started at any time of the menstrual cycle avoiding long delays in treatment.
SUCCESS RATES
When ready to attempt pregnancy, the frozen embryos are thawed and transferred to the uterus of the patient or, in some cases, a surrogate/gestational carrier in case the patient uterus is compromised. Embryo freezing is a highly successful technique that has been in use for more than 25 years. Live Birth rates for frozen embryo cycles range from 35-45% for women under 35.
POTENTIAL RISKS/CONCERNS WITH OVARIAN STIMULATION
- There is a risk with the use of injectable hormones for ovarian stimulation that they can lead to ovarian enlargement and hyper stimulation (OHSS).
- The need to delay the start of chemotherapy to allow for controlled ovarian stimulation of the ovaries. However, protocols can be used where stimulation begins in the luteal (second half) of the menstrual cycle and may provide a more flexible schedule for the utilization of hormonal stimulation
- Cost of treatment can also be a potential barrier.
C. OVARIAN SUPPRESSION (GnRH Agonists)
Ovarian suppression involves the use of GnRH agonists (e.g, leuprolide, goserelin) to decrease the effect of chemotherapy on the depletion of follicles appears to be a promising option in some cancers like breast cancer. GnRH agonist is administered by injections either monthly or every three months. It should be started around two to four weeks before the first chemotherapy treatment and continued throughout the duration of treatment.
Recently, the POEMS trial in Triple negative breast cancer patients demonstrated a significant reduction in ovarian failure and also a significantly increased odds ratio for pregnancy.
SUCCESS RATES
Ovarian suppression is an upcoming new procedure. It has been studied primarily in women with breast cancer and lymphoma and results evaluating effectiveness in preserving fertility are conflicting and the retention of ovarian function is not guaranteed.
POTENTIAL RISKS/CONCERNS
This procedure can cause menopausal like symptoms, which may be intolerable for some patients; add-back therapy may alleviate some of these symptoms. Additionally, it can also decrease bone density but this is largely reversible.
D. OVARIAN TISSUE FREEZING
Ovarian Tissue Freezing Is Currently An Experimental Technique As Per ASRM Guidelines However It Is Extensively Used In Europe And Japan. It Involves Surgically Removing All Or A Part Of The Cortex Of The Ovary, Which Contains Thousands Of Resting Primordial Follicles. read more
POTENTIAL LIMITATIONS?
- Experimental procedure to be done in an IRB protocol setting.
- This is an invasive surgical procedure requiring anaesthesia.
- Potential to re-introduce cancerous cells, particularly in hematologic malignancies
E. PROTECTION OF OVARIAN FUNCTION/OVARIAN TRANSPOSITION
Ovarian transposition refers to a surgical repositioning of the ovaries outside the pelvic radiation treatment (RT) field to reduce ovarian exposure. Ovarian transposition is generally performed using a minimally invasive surgical procedure. Metal staples are placed around the ovaries in their new locations in order to assist treatment providers visualizing the ovaries, to avoid including them in the RT fields. This procedure should be performed before RT simulation.
SUCCESS RATES
The retention of ovarian function using ovarian transposition is not guaranteed and patients should be offered egg or embryo freezing before treatment if there are no medical contraindications. If the fallopian tubes are resected, the patient will not be able to conceive naturally. Instead the patient would need to undergo ovarian stimulation and trans-abdominal egg retrieval. Alternatively, ovaries may be re-positioned after finishing RT in order to place them back into the pelvis.
If the uterus is exposed to a high dose of radiation during treatment, the patient may not be able to carry a pregnancy herself and may have to use a gestational carrier.
Ovarian transposition will not protect the ovaries from the effects of systemic chemotherapy.
POTENTIAL RISKS/CONCERNS
This procedure carries risks for complications from anaesthesia and typical risks associated with any invasive procedure, including bleeding and infection.
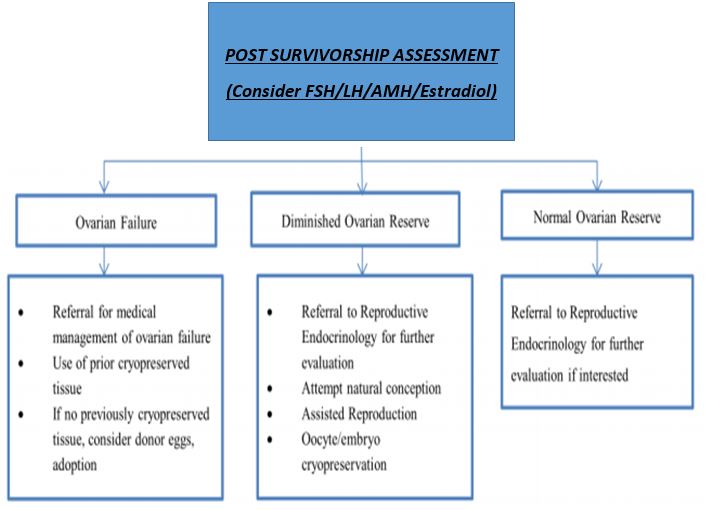
POST SURVIVORSHIP CARE
Evaluation by an endocrinologist is recommended, particularly as early ovarian failure can increase the risk for the development of osteoporosis and cardiovascular disease. The Childrens Oncology Group recommends that survivors at risk for infertility should be screened with measurements of LH, FSH and estradiol at age 13 and then as clinically indicated.
But, even with the addition of AMH and ovarian imaging it is not possible to correctly estimate the remaining duration of the reproductive window in a given individual.
Treatment Options Available For Male Child
Spermatogenesis, the process of maturation of spermatogonia (sperms) from spermatogonial stem cells (SSC), begins in puberty and then continues through a males lifetime.
Post pubertal males commonly experience temporary azoospermia during therapy as rapidly dividing spermatogonial cells are particularly sensitive to chemotherapy and radiation. SSC cells are less vulnerable to effects of gonadotoxic therapy but can still be affected. Permanent azoospermia therefore depends on the degree to which SSC are depleted, thus, pre-pubertal males are also at risk of permanent azoospermia
Moreover, surgical interventions that result in disruption of nerves supplying the reproductive organs may hamper chances of natural reproduction as well.
A. SPERM BANKING
Sperm banking is the freezing and storage of semen in post-pubertal boys at a sperm banking facility. Boys who are greater than Tanner stage III are usually mature enough to masturbate to ejaculation. Optimal procedures for the collection of sperm include abstinence 48 h prior to collection and the collection of multiple specimens, at least 24 h apart for cryopreservation. If the patient cannot ejaculate, alternative methods for sperm collection like electro-ejaculation, vibrator or medical methods can be used
Patients who can collect only a single specimen, and those who have low sperm counts or sperm with poor motility, should also sperm bank as there are new reproductive techniques to fertilize eggs. Once the specimen is frozen, it can be stored for many years, until the patient is ready to use.
A. POTENTIAL LIMITATIONS
- Inability to masturbate, whether secondary to age, illness or discomfort
- Electroejaculation (EEJ)-entails use of electrostimulation under general anaesthesia, however Sperm retrieval rates with EEJ average around 60% in the adolescent population.
- Surgical Sperm Retrieval-sperm may also be acquired surgically via epididymal sperm aspiration under local anaesthesia, or testicular sperm extraction (TESE) surgically under anaesthesia in cases where there is a obstructive azoospermia or in ability to masturbate.
FUTURE USE AND SUCCESS RATES
When ready to attempt pregnancy, the frozen semen specimens are thawed and a sperm analysis is done. The thawed specimen(s) is used with assisted reproductive technology procedures such as intrauterine insemination (IUI) or in vitro fertilization (IVF). Success rates vary based on age and fertility status of the female partner and on the quality of the pre-treatment specimen.
B. TESTICULAR TISSUE FREEZING TISSUE
Cryopreservation of testicular tissue that contains SSC offers an experimental option for preservation of fertility in pre-pubertal boys and post-pubertal males who cannot produce a sperm sample.
POTENTIAL LIMITATIONS
- No human applications for the use of thawed testicular tissue at present. Research is ongoing in animal models to develop maximally effective methods of freezing, thawing and transplanting this tissue.
- Experimental procedure to be done in an IRB protocol setting
- Concerns regarding the potential to re-introduce malignant cells.
C. PROTECTION OF TESTIS /TESTICULAR SHEILDING
Testicular shielding involves the placement of shields over the scrotal sac to reduce scatter radiation to testicular exposure. Clamshell-like shields are made during simulation and used each day of treatment with pelvic or inguinal radiation therapy. Intensity modulated radiation therapy (IMRT) may be used to minimize exposure in addition to or instead of shielding.
SUCCESS RATES
Shielding reduces radiation dose to the testes by 3x-10x. The farther the shielded testicle from the edge of the target area of radiation, the greater the reduction in damage from radiation.
D. NERVE SPARING SURGERIES
Some cancer surgeries involve the removal of lymph nodes in the abdomen (retroperitoneal lymph node dissection [RPLND]), and these surgeries can damage the nerves involved in ejaculation. While this does not cause a male to be infertile, it does mean that, when ready to attempt pregnancy, sperm has to be retrieved in other ways. Nerve-sparing RPLND techniques should be discussed with appropriate patients, especially those interested in future fertility.


CONCLUSIONS
With excellent survival rates and advances in the field of Onco-ART, fertility preservation in the paediatric and adolescent patients diagnosed with cancer is an important component of comprehensive care and allows these survivors to have their own biological children.
